Neonatal Quality Improvement
Neonatal Quality Improvement 4
744 - Decreasing Iatrogenic Anemia in the NICU
Publication Number: 744.343

Lisa R. Jasin, DNP NNP-BC
Neonatal Nurse Practitioner
Dayton Children's Hospital
Dayton, Ohio, United States
Presenting Author(s)
Background:
In a pediatric teaching hospital Neonatal Intensive Care Unit (NICU) "routine" lab testing in the NICU was ordered two days per week for all newly admitted patients. Nurses and phlebotomists did not have a standardized volume to obtain for each ordered lab test. This led to infant labs drawn, at times, without medical indication. Blood loss for laboratory tests in the neonate may lead to an increase in packed red blood cell transfusions.
Objective: The aim of the project was to decrease the average volume of blood that was drawn weekly from premature babies with a birthweight less than 2000 grams in the NICU.
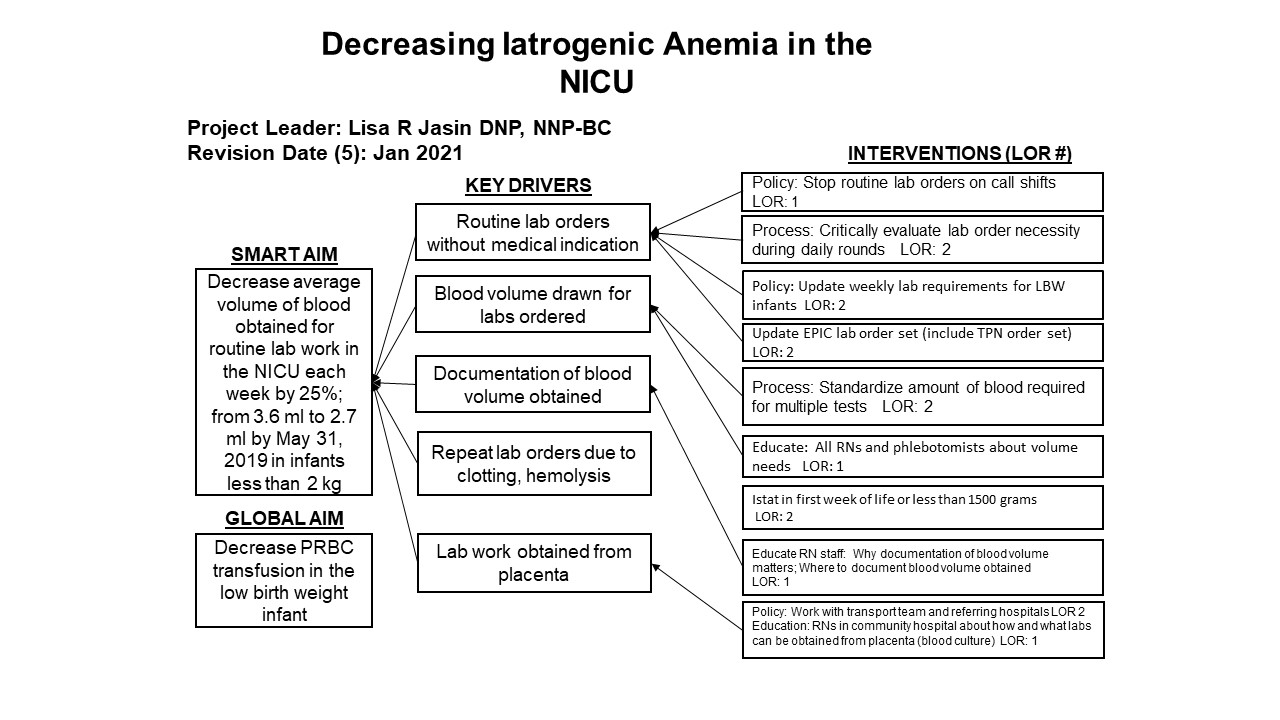
Design/Methods: The Institute for Healthcare Improvement (IHI) Model for Improvement framed the project. A Key Driver Diagram guided implementation of Plan-Do-Study-Act (PDSA) cycles to test changes in discussions of ordered labs on daily interdisciplinary family centered NICU rounds, daily sign out between providers, and standardization of expiration of routine lab work on all newly admitted infants. A run chart was used to follow outcomes and determine significant changes in average blood volume drawn weekly and average hemoglobin in infants less than 2000 grams in the NICU. A threshold of 8 points above or below the median was used to indicate a change. Data was collected weekly on all infants with a birthweight below 2000 grams until discharge. Only infants who had labs drawn were included in the weekly denominator so as not to artificially lower the average volume of blood drawn.
Results:
There was an initial weekly mean average blood volume drawn of 3.6 ml. Initial interventions led to a decrease in the mean volume to 1.8 ml of blood drawn. As PDSA cycles progressed, the mean increased to 3.6 ml, and later decreased to 1.6 ml, exceeding the goal of 2.7 ml average blood volume. Monthly monitoring showed a further decrease to 1.2 ml that has been sustained for over 2 years. There was a statistically significant increase in infants' average hemoglobin from 10.2 to 11.34 g/dL.
Conclusion(s): The plan for sustainability was built into the key driver diagram. Routine lab orders can be replaced with medically indicated lab draws. The order set was changed in the electronic medical record to assist in ordering the appropriate labs. The electronic orders have a defined stop date so the orders do not continue in perpetuity. A laminated card has been placed at each workstation to provide ordering guidance. Review of labs ordered is now a permanent part of family centered rounds. Discussion of labs ordered is a part of shift handoff. 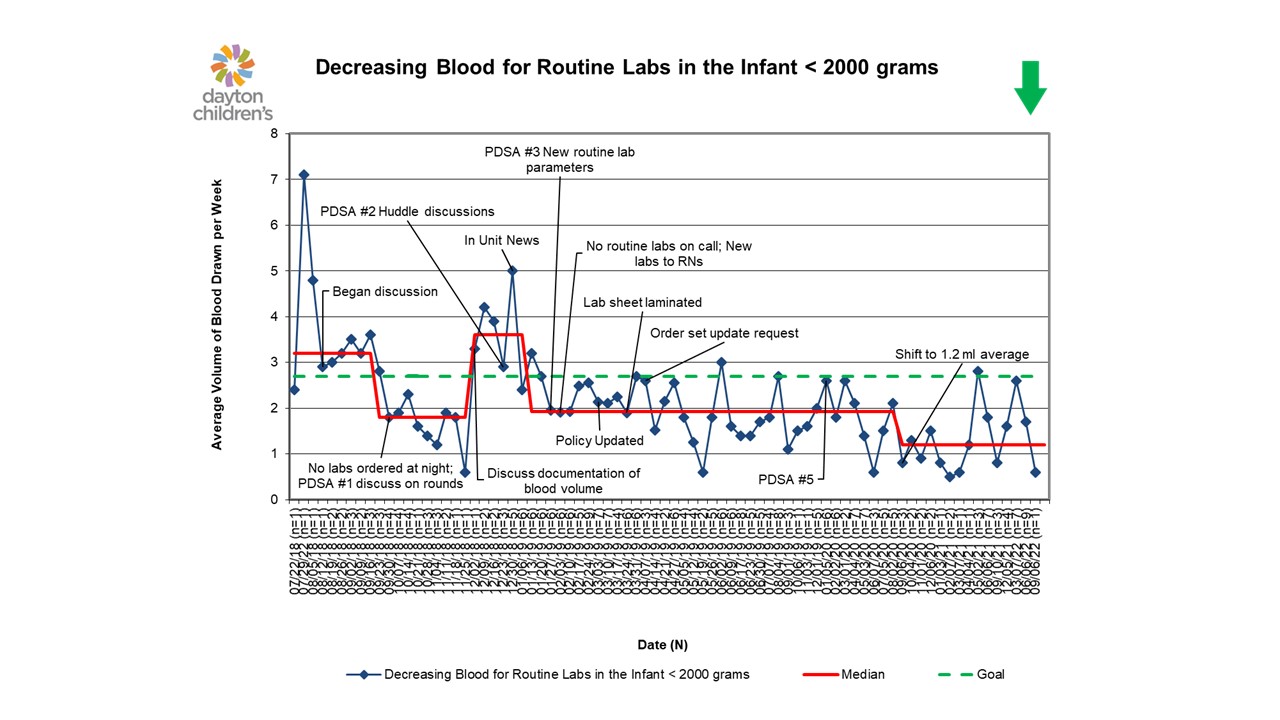
.jpg)
