Emergency Medicine: Quality Improvement
Emergency Medicine 10
472 - Use of Core Medication Teaching Elements at ED Discharge Differs by Staff Role
Publication Number: 472.309

Austin Gerdes, MPH (he/him/his)
Medical Student
Medical College of Wisconsin
Greenfield, Wisconsin, United States
Presenting Author(s)
Background:
Caregivers often mis-dose medication causing harm and utilization of healthcare. In the pediatric emergency department (PED), high quality medication teaching is vital to preventing harm. Many evidence-based medication teaching best practices exist. However, few Quality Improvement (QI) efforts have focused on medication teaching.
Objective:
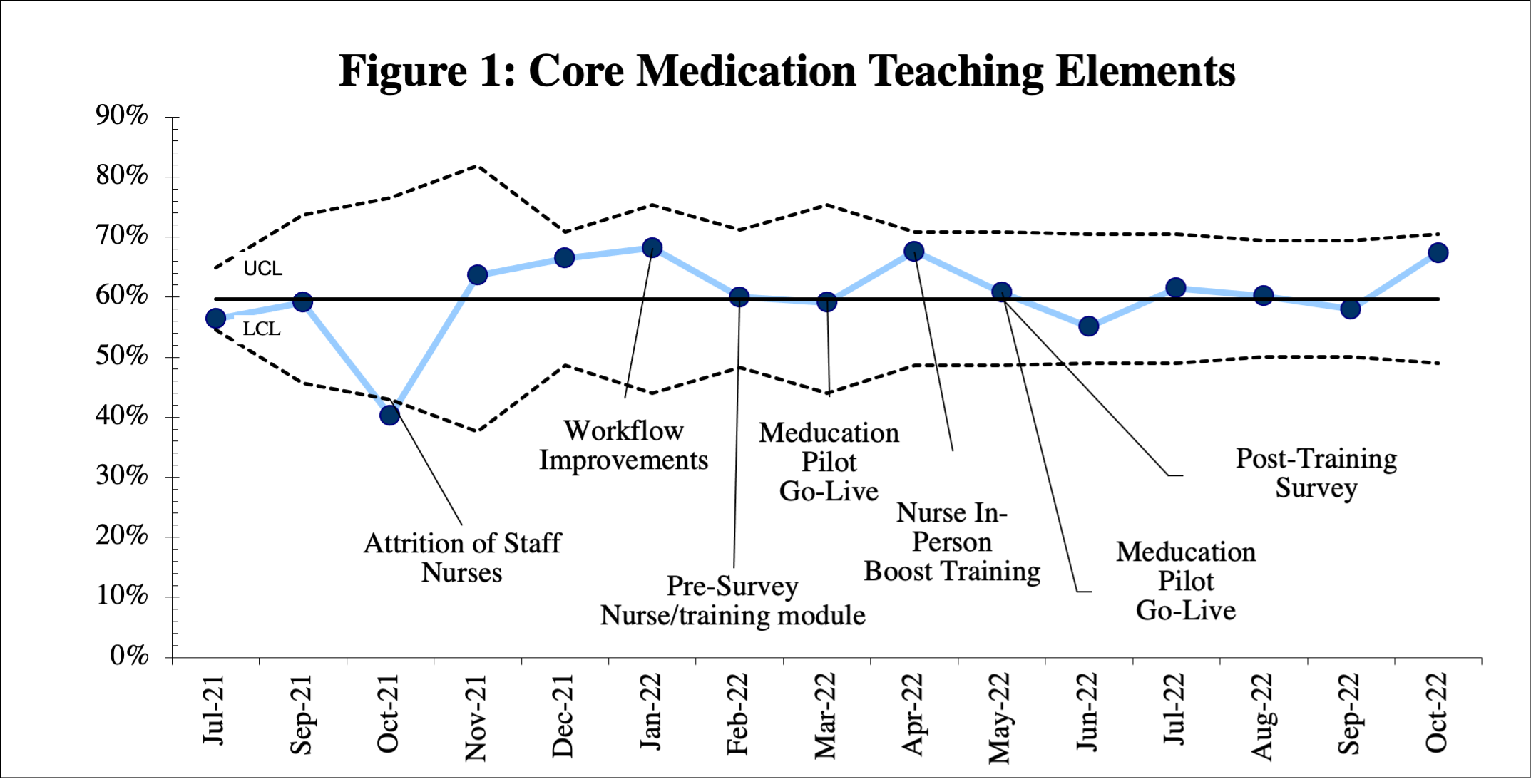
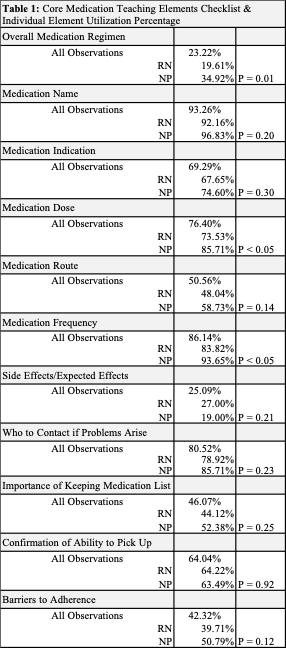
To improve the percentage of ED discharges with core medication teaching elements (Table 1) covered during discharge teaching.
Design/Methods:
An improvement team determined key drivers of patients receiving quality discharge medication teaching. Workflow diagrams, value stream map, and cause and effect diagrams aided in planning. Interventions included workflow improvement, physician, APP, and nursing training on best practices, improvements in the EHR discharge tools, and boost trainings at staff meetings.
A discharge observation checklist, including discharging staff role and core medication teaching elements, was completed by a trained observer. Analysis included the percentage of each element as well as all elements as an overall percentage of the checklist completed. The percent of discharges with the technique completed were followed on run and statistical process control charts (p-charts). Chi-square tests were used to compare the proportions of Nurse vs. NP completing discharge elements.
Results:
A total of 267 discharges were observed and evaluated using the developed core medication teaching elements checklist. During the implementation period, a “Helping Hands” program, consisting of mainly NPs, began to aid with discharges in a high turnover areas of the ED during times of staff attrition and high ED volumes. A total of 204 discharges by RNs and 63 by NPs were observed. Overall, the core medication teaching elements were completed on average 57.2% of the time. There was no special cause noted over time during the study period (Figure 1).
When comparing RNs vs the NPs in the discharge specific role, NPs were found to teach the overall medication regimen (35% vs 20%), medication dose (85% vs 73%) and frequency (94% vs 85%) significantly more than staff nurses (p< 0.05 for all, Table 1).
Conclusion(s):
There was no significant increase in the core medication teaching elements over time. There were differences by staff teaching role (RN vs NP) with each demonstrating different strengths in medication teaching. This not only serves as evidence for the importance of interdisciplinary teaching, but also demonstrates the need for role clarity and ensuring staff have the time and tools needed for safe ED discharge.