Back
Background: Clinical trials have demonstrated that compared to the nebulized route, β-agonist bronchodilators given via Metered Dose Inhalers and Dexamethasone used as preferred steroids are non-inferior to traditional Asthma treatment. We implemented evidence-based Asthma Pathways in our institute and initiated a QI project with PDSA cycles to improve the quality of Asthma care.
Objective: Our objective was to reduce the median length of stay by 20%, and 7 and 30 days readmission rates by 5% for patients hospitalized for an Acute Asthma Exacerbation at the Nemours Children’s Hospital. We encouraged adherence to the Asthma Pathway as well as the use of Albuterol MDI and Dexamethasone.
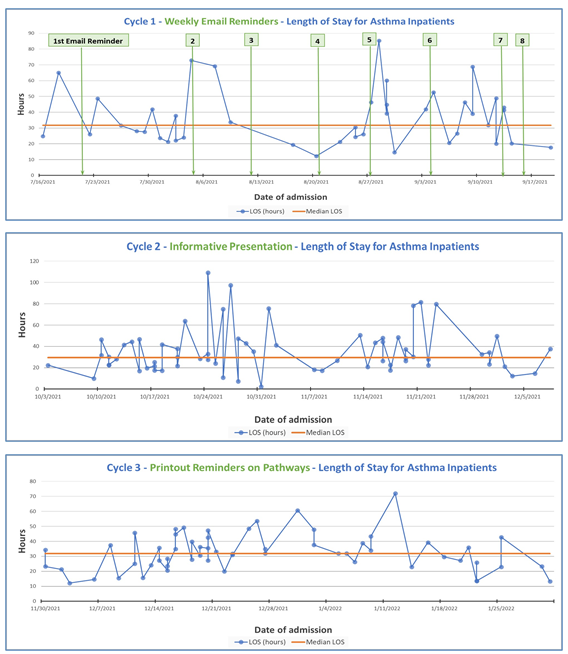
Design/Methods: A quality improvement project with PDSA cycles was initiated for hospitalized patients between July 2021 till Feb 2022 with acute Asthma exacerbations. PICU patients were not included. Evidence-based Asthma pathways were created with specific inclusion and exclusion criteria. Baseline data were obtained from EMR a year prior to the study from July 2020 to June 2021. The process measure included three tests of change implemented for 8 weeks each, and data was collected from EMR on a weekly basis to document readmission rates and length of stay. The outcome measures tracked were readmission rates and median length of stay. Compliance with MDI and Dexamethasone was also tracked. The first PDSA cycle included a test of change with weekly email reminders to the providers and sharing data with them, the second PDSA cycle was an oral presentation for residents and the hospitalist team separately but on the same day, and the third PDSA cycle was placing color printouts of pathways in strategic locations. The balancing measure was the limitation of manpower in the pharmacy to dispense MDI.
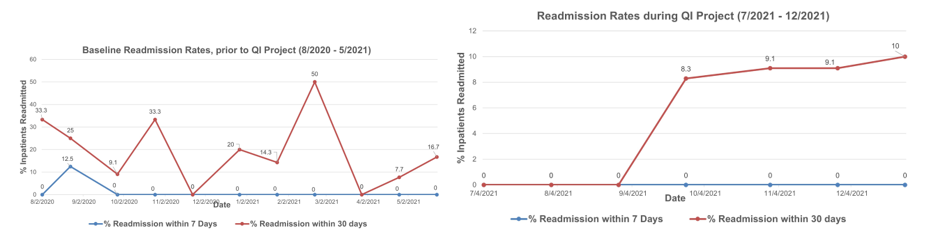
Results: Baseline data prior to the implementation of Asthma pathways from July 2020 - June 2021 included 283 patients that showed a median LOS of 44.75 hours, with 7 days and 30 days readmission rates of 1.3% and 13.9% respectively. Our collected data of 174 patients from July 2021-Feb 2022 during PDSA cycles showed improvements with a median LOS decreased to 31.8 hours and 7 days and 30 days readmission rates were 0% and 5.7% respectively. Adherence to MDI and Dexamethasone use was 92.5% and 85.6 % respectively.
Conclusion(s): Implementation of evidence-based Asthma pathways and adherence to the use of Albuterol MDI and Dexamethasone as preferred corticosteroids can reduce the median length of stay and readmission rates of patients hospitalized for Asthma exacerbation.
.png)
Asthma
Asthma 1
360 - Improved quality of Asthma care by implementing Asthma Pathways, administering Albuterol via metered dose inhaler and using Dexamethasone as preferred steroids.
Sunday, April 30, 2023
3:30 PM – 6:00 PM ET
Poster Number: 360
Publication Number: 360.302
Publication Number: 360.302
Syed A. Ali, Nemours Children's Hospital, Saint Cloud, FL, United States; Adam Talaat, University of Central Florida College of Medicine, Orlando, FL, United States

Adam Talaat
Medical Student
University of Central Florida College of Medicine
Orlando, Florida, United States- SA
Syed A. Ali, MD
Pediatric Hospitalist
Nemours Children's Hospital
Saint Cloud, Florida, United States
Presenting Author(s)
Co-Author(s)
Background: Clinical trials have demonstrated that compared to the nebulized route, β-agonist bronchodilators given via Metered Dose Inhalers and Dexamethasone used as preferred steroids are non-inferior to traditional Asthma treatment. We implemented evidence-based Asthma Pathways in our institute and initiated a QI project with PDSA cycles to improve the quality of Asthma care.
Objective: Our objective was to reduce the median length of stay by 20%, and 7 and 30 days readmission rates by 5% for patients hospitalized for an Acute Asthma Exacerbation at the Nemours Children’s Hospital. We encouraged adherence to the Asthma Pathway as well as the use of Albuterol MDI and Dexamethasone.
Design/Methods: A quality improvement project with PDSA cycles was initiated for hospitalized patients between July 2021 till Feb 2022 with acute Asthma exacerbations. PICU patients were not included. Evidence-based Asthma pathways were created with specific inclusion and exclusion criteria. Baseline data were obtained from EMR a year prior to the study from July 2020 to June 2021. The process measure included three tests of change implemented for 8 weeks each, and data was collected from EMR on a weekly basis to document readmission rates and length of stay. The outcome measures tracked were readmission rates and median length of stay. Compliance with MDI and Dexamethasone was also tracked. The first PDSA cycle included a test of change with weekly email reminders to the providers and sharing data with them, the second PDSA cycle was an oral presentation for residents and the hospitalist team separately but on the same day, and the third PDSA cycle was placing color printouts of pathways in strategic locations. The balancing measure was the limitation of manpower in the pharmacy to dispense MDI.
Results: Baseline data prior to the implementation of Asthma pathways from July 2020 - June 2021 included 283 patients that showed a median LOS of 44.75 hours, with 7 days and 30 days readmission rates of 1.3% and 13.9% respectively. Our collected data of 174 patients from July 2021-Feb 2022 during PDSA cycles showed improvements with a median LOS decreased to 31.8 hours and 7 days and 30 days readmission rates were 0% and 5.7% respectively. Adherence to MDI and Dexamethasone use was 92.5% and 85.6 % respectively.
Conclusion(s): Implementation of evidence-based Asthma pathways and adherence to the use of Albuterol MDI and Dexamethasone as preferred corticosteroids can reduce the median length of stay and readmission rates of patients hospitalized for Asthma exacerbation.


.png)
